Trust, State Capacity, and Administrative Burden in Pakistan’s Immunization Program
Vaccine hesitancy is a global phenomenon and one of particular concern at the present moment with the deployment of COVID-19 vaccines and their reception around the world. An extensive literature studies the characteristics that correlate with hesitancy and refusals, such as maternal education, religious views, gaps in capacity, and service provision. In this brief article, we begin with the premise that immunization is a site of interaction between the state and its citizens. Relying on work from sociology and public administration, specifically the administrative burden framework, we argue that the context in which this interaction takes place, and the costs it imposes on citizens, is crucial to attitudes toward vaccination.
Sociological work on understanding parental medical choices highlights the need to explore the “priorities, processes, and ambivalences” that inform decision-making. Vaccination programs are situations where a representative of the state initiates contact with the citizen, similarly to a census or voter identification exercise. In developing countries like Pakistan, these encounters mean that a state that is often absent knocks at the citizen’s door to offer a service free of charge. As such, conventional modes of citizen “claim-making” are turned on their head. Therefore, immunization programs are a test of a citizen’s trust in the state and its functionaries and are revelatory of state capacity. These factors, in turn, shape parental perception of costs associated with government run vaccination programs, specifically, “the learning, psychological, and compliance costs that citizens experience in their interactions with government”; that is, administrative burdens.
Context and Methods
We investigate the implementation of immunization programs in Pakistan, a Low- to Middle-Income Country (LMIC), detailing how distrust in the state and low administrative capacity exacerbate the learning, psychological, and compliance costs citizens experience in their interactions with state representatives.
Pakistan is ranked third for the most un- or under-immunized children, with an infant mortality rate of 69 per 1000 births—the highest in South Asia. The country receives considerable funding for immunization programming and procurement through Pakistan’s Expanded Program for Immunization (EPI), and yet vaccine preventable diseases persist, including polio. There is considerable regional variation in disease incidence, aligning with patterns of socio-economic inequality and literacy. A great deal has been written on why Pakistan is unable to ensure greater vaccination coverage, with explanations ranging from corruption, unplanned devolution, and poor access to services to religious beliefs and lack of awareness.
We conducted over a year of mixed methods research, including an exploratory survey and qualitative fieldwork (semi-participant observations at government hospitals and selected BHUs and RHCs, and interviews) designed to understand issues in the supply and demand of immunization services in Kasur, Punjab, a relatively well-developed district neighbouring Lahore. We surveyed 179 households across the district of Kasur and drew on data from the Pakistan Social and Living Standard Measurement (PSLM) Surveys 2012-13 and 2014-15. Of those surveyed, two-thirds had their children’s vaccination booklet to hand. Of the children in our sample households, 195 had a unique vaccination record booklet available. We photographed the record page of these booklets (without collecting any identifying information) and found that 73% were fully vaccinated for their age group—government data estimates 75% of children are fully immunized at 12-23 months in Kasur (PHS 2016). Our tabulation of records revealed that 16% had experienced a delay in some vaccinations (though overall their record was accurate for their age), while 27% had missed doses of some vaccines.

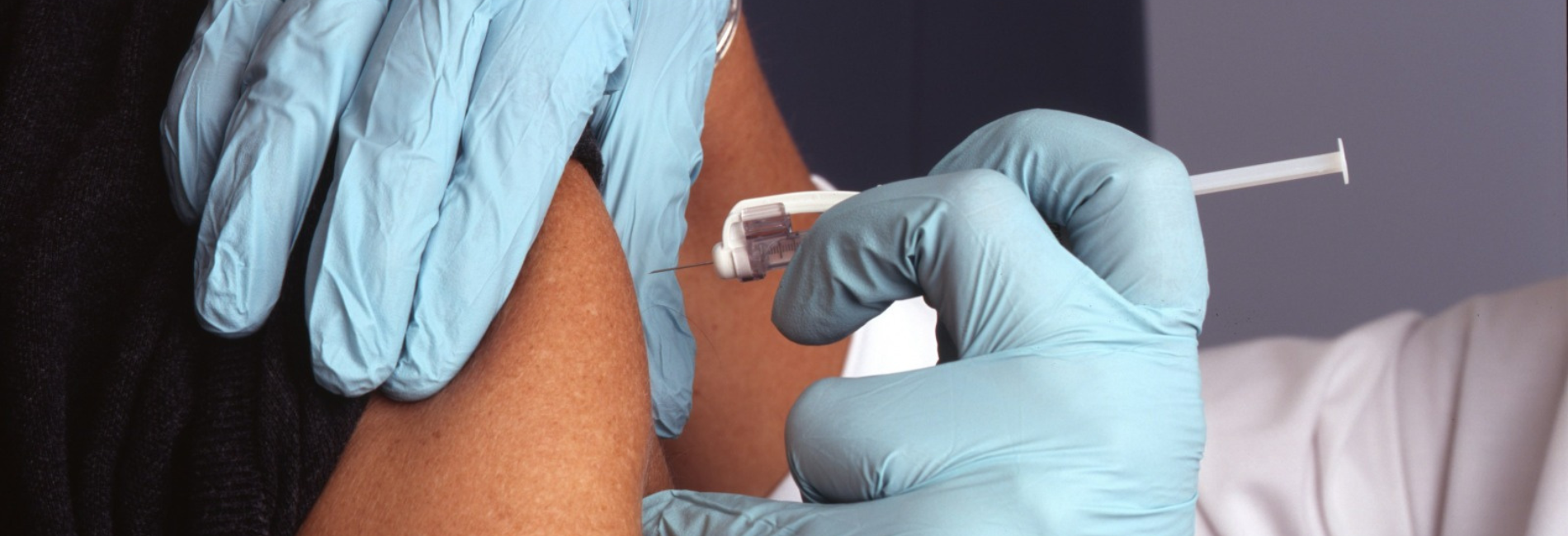
Image 1: Child vaccination booklet
Source: Authors
Encounters with the State
Over the past few years, communities in the former Federally Administered Tribal Areas (FATA), now the Newly Merged Districts (NMDs) of Khyber Pakhtunkhwa province of Pakistan—where the state has been largely absent or coercive—are using the polio vaccine as a bargaining chip to gain concessions from the state. These tactics are not unique to Pakistan but Pakistan’s immunization program has struggled to adapt programming to different contexts and learn from tactics other countries have adopted. Fundamental to such adaptation is the recognition that encounters over immunization are shaped by prior experience with, and perception of, the state and its representatives. Even in Kasur, located in the country’s most developed province (the Punjab), some of our respondents feared that the objective of our survey was so that the government could impose new taxes on them based on the number of children they had.
Such perceptions are critically important because vaccines are administered when children are not symptomatic. This imposes considerable learning, compliance, and psychological costs on parents who feel responsible for their children’s health and well-being. In many cases, parents have reasonable concerns about cold chain maintenance, spurious medications, and expiry dates. Though the majority of our respondents believed vaccines to be safe and effective, two-thirds of them claimed that the vaccinator did not explain how vaccines work, and they did not ask the vaccinator to explain. The lack of interaction with frontline workers is alarming considering that just 37% were aware of minor side effects of vaccines (fever, soreness), and most respondents were not aware that vaccines are available for diseases other than polio. One mother explained her refusal to vaccinate:
“She had fever for three days after she got the injections, normally the fever lasts only a few hours after the injection. Her fever lasted three days, so we didn’t get her vaccinated the next time.”
In such situations, the role of frontline health workers is critical during immunization campaigns in overcoming hesitancy, addressing disinformation, and counteracting refusals. However, overburdened staff are usually not able to dedicate the time and resources required to address parents’ concerns due to capacity constraints, and can come across as harsh, dismissive, and judgemental. Respondents told us:
“They inform us of only the repercussions of not getting the child vaccinated for polio; they don’t give us proper details about the whole process and why it is important. The information we have is through television; the LHW doesn’t provide us with the full details.”
As the population has grown, staffing and planning have both failed to keep pace. Vaccinators struggle to vaccinate all eligible children but are very aware of targets set by the department that must be met. As a result of capacity limitations, the learning, psychological, and compliance costs once again shift to the parent—not all of whom have the capacity to handle these additional burdens.
Effectively then, distrust in the state and low administrative capacity significantly augments administrative burdens on citizens since they must look elsewhere for support. The consequence is a considerable amount of stress for parents as they must navigate state encounters and parental responsibility. In the face of learning, psychological, and compliance costs, parents often turn to private health care facilities where they might find staff to be more attentive and available. The reliance on private health care in Pakistan is growing and is a poor reflection on state service provision. Improving healthcare facilities is not simply a matter of financial investment or infrastructure, but a fundamentally political exercise that needs to centre the citizen’s experience of the state. The pandemic provides an opportunity for Pakistan’s policymakers to correct course, and enhance responsiveness to citizen needs; it remains to be seen if they will take advantage of it.
Sameen A. Mohsin Ali is Assistant Professor at the Mushtaq Gurmani School of Humanities and Social Sciences, LUMS
Samia W. Altaf is Professor of Practice in Public Health, LUMS.
Mahbub ul Haq Research Centre at LUMS
Postal Address
LUMS
Sector U, DHA
Lahore Cantt, 54792, Pakistan
Office Hours
Mon. to Fri., 8:30 a.m. to 5:00 p.m.